- By Priyanka Munshi
- Thu, 09 May 2024 02:09 PM (IST)
- Source:JND
Did you know that genetics can play a role in ovarian cancer risk? Specific gene abnormalities can increase susceptibility. Ovarian cancer risk is significantly influenced by the BRCA1 and BRCA2 genes, which are commonly linked to breast cancer. Compared to women without mutations, females carrying these gene alterations are more likely to develop ovarian cancer.
Furthermore, Lynch syndrome, a hereditary disorder caused by mutations in genes involved in DNA repair, may increase the risk of ovarian cancer. By using testing to determine one's genetic susceptibility, people can take control of their healthcare decisions by utilizing early detection and preventive treatments. In a conversation with Jagran English, Dr. Kunjal Lila, Head of Department and Consultant in Surgical Pathology at Metropolis Healthcare Ltd., talked about how genetics can be a risk factor for ovarian cancer.
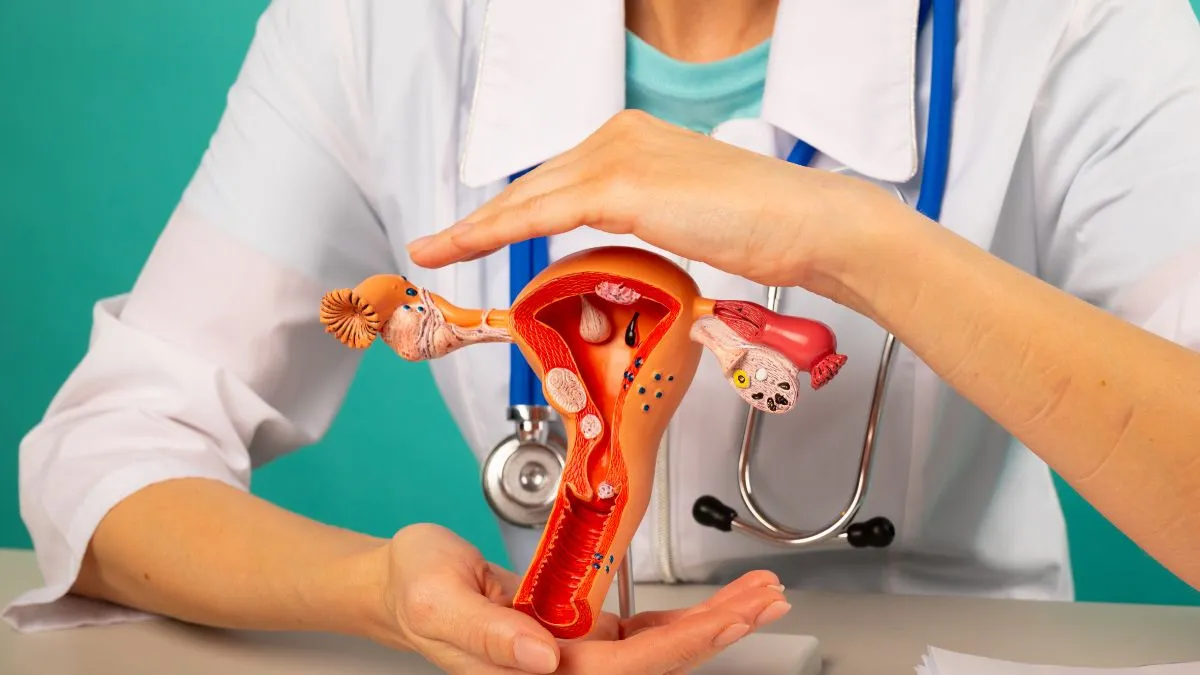
Ovaries are a pair of glands that produce eggs and female hormones. Ovarian cancer is a type of cancer that begins in the ovaries. It is one of the leading causes of cancer deaths among women. Various risk factors are implicated in its genesis. The non-genetic ones include age (over the age of 63), obesity, late pregnancy after 35 years of age, hormone therapy after menopause, smoking, assisted reproductive therapies, etc.
According to Dr. Kunjal, as per the Ovarian Cancer Research Alliance (OCRA), about 20–25% of women with ovarian cancer have a hereditary or genetic tendency to develop the disease. This means that these cancers tend to run in families and there is a chance that siblings and children can also develop cancer, not only of the ovary but also of other organs like the breast, colon, pancreas, prostate, etc. The most significant genetic risk factor for ovarian cancer is an inherited mutation in breast cancer genes (BRCA1 or BRCA2), responsible for 10-15% of ovarian cancers. It is linked to both breast and ovarian cancers and is hence called Hereditary Breast and Ovarian Cancer Syndrome (HBOC). As per data from the National Cancer Institute, 39–44% of women with a harmful BRCA1 variant and 11–17% of women with a harmful BRCA2 variant will develop ovarian cancer.
Another genetic syndrome associated with hereditary ovarian cancers is Lynch syndrome (Hereditary Non-Polyposis Colorectal Cancer, or HNPCC), with an associated risk of colonic and uterine cancers. Various studies show germline mutations in other genes as possible risk factors for ovarian cancer, with scientists still discovering more culprits. Having said this, some clues may point towards the genetic origin of ovarian cancer. These include a personal history of cancer before age 40, a family history of ovarian, breast, uterine, or colon cancers, a first-degree relative (mother, sister, or daughter) with ovarian cancer, two or more close relatives with breast cancer before age 50, or ovarian cancer at any age.

Lynch syndrome, a hereditary disorder, can also increase the risk of ovarian cancer.(Image Credit:Canva)
Dr. Kunjal emphasised that all these factors should compel us to prioritize genetic testing. It's crucial to note that cancer affects not only females but also males, particularly prostate and pancreatic cancers. Genetic testing, when accompanied by comprehensive pre- and post-test genetic counseling, empowers individuals to take proactive measures to reduce their cancer risk or detect it at an early stage. Moreover, it plays a pivotal role in guiding treatment decisions not only for the affected individual but also for other family members who may be at risk.

Early detection and preventive treatments can be achieved through genetic testing.(Image Credit:Canva)
Lastly, Dr. Kunjal suggested that incorporating genetic testing and counseling into our healthcare practices can significantly improve outcomes by enabling personalized prevention strategies and tailored treatment plans.